Neuropathic pain results from nerve damage or dysfunction, manifesting as burning, tingling, or shooting sensations, and can be effectively managed through a combination of medication, physical therapy, lifestyle changes, and early diagnosis.
Neuropathic pain: causes and treatments can significantly impact your quality of life. Have you ever dealt with persistent, sharp pain that seems to come out of nowhere? Identifying the roots of such discomfort and finding effective treatments is crucial to regaining control.
What is neuropathic pain?
Neuropathic pain is a type of pain that occurs when nerve fibers are damaged, dysfunctional, or injured. This type of pain can be persistent and difficult to treat. It often feels different from other kinds of pain, such as acute pain, which is caused by injury or illness. People may describe neuropathic pain as burning, tingling, or electrical sensations.
The causes of neuropathic pain can be varied. Conditions such as diabetes, multiple sclerosis, shingles, and certain injuries can lead to nerve damage. Diabetic neuropathy is one common example where high blood sugar levels cause nerve damage over time.
Symptoms of Neuropathic Pain
Symptoms can include sharp, shooting pain, sensitivity to touch, and a feeling of numbness or weakness in the affected area. Some individuals may also experience pain without a clear cause. This can be incredibly frustrating and challenging.
Diagnosis of neuropathic pain often involves a combination of physical exams, patient history, and sometimes nerve conduction studies. A healthcare provider may ask about the severity and type of pain to better understand the condition.
Understanding neuropathic pain is essential for effective management and treatment. By identifying the underlying cause, healthcare professionals can suggest appropriate therapies and strategies to help alleviate symptoms and improve quality of life.
Common causes of neuropathic pain
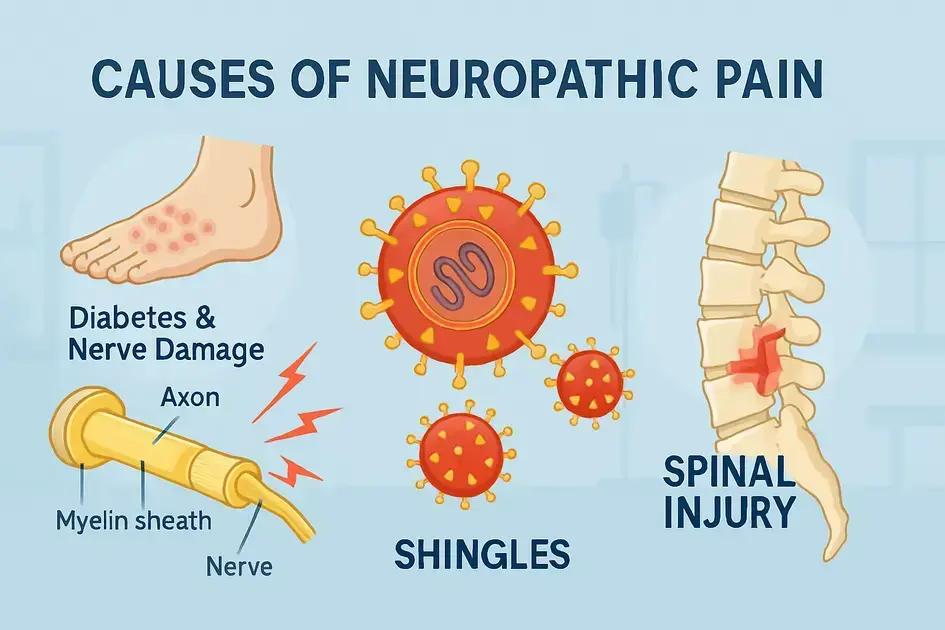
There are several common causes of neuropathic pain, each leading to nerve damage or dysfunction. One of the primary causes is diabetes. Diabetic neuropathy occurs when high blood sugar levels damage the nerves over time, often causing pain and numbness in the legs and feet.
Another significant cause is herpes zoster, commonly known as shingles. This viral infection can lead to nerve pain even after the rash has healed. The pain associated with shingles may last long after the initial illness.
Multiple sclerosis is also linked with neuropathic pain. This chronic condition affects the nervous system, leading to various symptoms, including nerve pain. Because it disrupts the communication between the brain and the body, those with multiple sclerosis may experience various types of nerve-related pain.
Injuries, particularly those involving the spine, can lead to neuropathic pain by damaging spinal nerves. This includes accidents or falls that cause trauma to the back or neck areas.
Additionally, alcohol abuse can also harm nerves, leading to alcoholic neuropathy. This condition can result in pain, weakness, or numbness, especially in the legs and hands.
Certain medical conditions, such as autoimmune diseases and thyroid issues, can also predispose individuals to neuropathic pain. These conditions may interfere with nerve function and contribute to pain sensations.
Understanding the specific cause of neuropathic pain is crucial for effective treatment and management. Identifying these underlying conditions can help healthcare providers recommend appropriate therapies.
Symptoms associated with neuropathic pain
Symptoms associated with neuropathic pain can vary widely among individuals, making it essential to understand what to look for. One of the most common symptoms is a burning sensation, which can feel like intense heat in the affected area.
Another frequent symptom is tingling or a “pins and needles” feeling, known as paresthesia. This sensation can be mild or severe and may come and go unpredictably.
Some individuals experience sudden, sharp pain that can feel like an electric shock. This type of pain can be triggered by touch, movement, or even changes in temperature. It often interrupts daily activities and can be alarming.
Numbness is also a common symptom, making it challenging to feel sensations in the affected area. This can lead to further complications, like injuries, since individuals may not realize they are hurting themselves.
In many cases, neuropathic pain can be accompanied by increased sensitivity to external stimuli. For example, pressure from clothing or a light touch may cause pain, a condition known as allodynia.
The intensity and combination of these symptoms can vary greatly. Some may experience mild discomfort, while others may find that their quality of life is significantly affected. Early recognition of these symptoms can help lead to timely and effective treatment.
If you or someone you know is experiencing these symptoms, it is important to consult a healthcare provider for an accurate diagnosis and appropriate management.
How neuropathic pain differs from other pain types

Neuropathic pain differs from other types of pain, such as nociceptive pain, in several important ways. Nociceptive pain is typically caused by physical injury or inflammation. For example, if you hurt your ankle, the pain comes from the injury itself and the body’s response to it.
On the other hand, neuropathic pain arises from nerve damage or dysfunction. It does not always correlate with an external injury. Instead, the nervous system malfunctions, sending pain signals even when there is no actual damage present.
Another significant difference is how the pain feels. Nociceptive pain is often described as sharp, aching, or throbbing, while neuropathic pain can feel like burning, tingling, or shooting sensations. This distinctiveness makes neuropathic pain particularly challenging to diagnose and treat.
Neuropathic pain can also occur alongside other pain types. For instance, someone could experience nociceptive pain due to a broken leg and then develop neuropathic pain from nerve damage related to the injury.
Furthermore, the response to treatments can vary greatly between these pain types. Conventional pain relief methods, such as non-steroidal anti-inflammatory drugs (NSAIDs), may be effective for nociceptive pain but may not relieve neuropathic pain. Instead, neuropathic pain often requires specific treatments, such as anticonvulsants or antidepressants.
Recognizing these differences is crucial for effective pain management. Understanding whether pain is neuropathic or nociceptive helps healthcare providers create tailored treatment plans to address the patient’s unique needs.
Potential risk factors for developing neuropathic pain
Several potential risk factors can contribute to the development of neuropathic pain. Understanding these factors is essential for prevention and management. One major risk factor is diabetes. Individuals with diabetes can experience high blood sugar levels, leading to nerve damage over time, known as diabetic neuropathy.
Another significant risk factor is age. As people get older, their nerves may naturally become more susceptible to damage. This can increase the likelihood of experiencing neuropathic pain.
Injuries to the spine or other areas can also increase the risk. Such injuries may cause nerve damage that leads to chronic pain conditions. Additionally, conditions like multiple sclerosis or HIV/AIDS can affect nerve function and contribute to neuropathic pain.
Other health issues, such as autoimmune diseases, can also pose a risk. These diseases may cause the body’s immune system to attack the nerves, resulting in pain and discomfort.
Alcohol abuse is another significant factor. Chronic alcohol consumption can lead to nerve damage, known as alcoholic neuropathy, which contributes to pain symptoms.
Lastly, certain medications, particularly chemotherapy drugs used in cancer treatment, can lead to neuropathic pain as a side effect. Understanding these risk factors can help individuals make informed choices to reduce their chances of developing neuropathic pain.
Effective treatments for neuropathic pain

Several effective treatments exist for managing neuropathic pain, tailored to address its unique causes and symptoms. One commonly used treatment is medication. Certain medications, such as antidepressants and anticonvulsants, have been shown to help reduce nerve pain. Drugs like gabapentin and pregabalin can modify the way the nervous system transmits pain signals, providing relief.
Another option is the use of topical treatments. Creams or patches containing medications like lidocaine or capsaicin can be applied directly to the skin over the painful area, helping alleviate localized discomfort.
Physical therapy is also a valuable treatment. A trained therapist can guide exercises that strengthen muscles and improve flexibility, which may help reduce pain and improve mobility. This approach focuses on restoring function and reducing symptoms.
For those who do not find relief from medication or physical therapy, nerve blocks or injections may be considered. These procedures involve injecting medication near a specific nerve to interrupt pain signals.
Additionally, some individuals find benefit from alternative therapies like acupuncture or yoga. These practices can promote relaxation and improve overall well-being, potentially helping with pain management.
It is essential for patients to work closely with their healthcare provider to determine the most appropriate treatment plan. Addressing the individual’s specific symptoms and health needs can lead to better management of neuropathic pain.
Medications for managing neuropathic pain
When it comes to managing neuropathic pain, various medications can be effective. Understanding these options is crucial for patients seeking relief. One of the most common types of medications is antidepressants, particularly tricyclic antidepressants like amitriptyline and nortriptyline. These can help reduce nerve pain by altering the way the brain processes pain signals.
Anticonvulsants are another class of medications that can be beneficial for neuropathic pain. Drugs such as gabapentin and pregabalin work by stabilizing nerve activity and reducing pain. They are often prescribed specifically for pain conditions linked to nerve issues.
In some cases, opioids may be considered for short-term use. While they are powerful pain relievers, they are usually not the first choice due to the risk of dependency and side effects. It is essential that they are prescribed and monitored closely by a healthcare professional.
Topical treatments can also play a role in managing neuropathic pain. Medications like lidocaine patches and capsaicin cream can be applied directly to painful areas, providing localized relief without significant systemic effects.
Additionally, other options like NSAIDs (non-steroidal anti-inflammatory drugs) may help address inflammation that could contribute to pain, although they are not specifically targeted at neuropathic pain.
It’s important for patients to work closely with their healthcare providers to determine the best medication plan based on individual needs and medical history. This personalized approach helps maximize pain relief while minimizing potential side effects.
Physical therapy techniques for relief

Physical therapy plays a significant role in managing neuropathic pain. Various techniques can help relieve pain and improve function. One effective approach is manual therapy. This involves hands-on techniques to mobilize soft tissues and joints, promoting blood flow and reducing tension in affected areas.
Therapeutic exercises are another important aspect of physical therapy. These exercises are tailored to an individual’s specific needs and help strengthen muscles, improve flexibility, and increase range of motion. Gradual progression of these exercises can lead to better overall physical function.
Electrical stimulation is a technique frequently used in physical therapy. It involves using devices that deliver small electrical impulses to stimulate nerves and muscles, which can help reduce pain and promote healing. For some, this method can provide significant relief from persistent pain.
Heat and cold therapy are simple yet effective techniques used to manage neuropathic pain. Applying heat can relax tense muscles and improve blood circulation, while cold therapy can numb the pain and reduce inflammation.
Additionally, educational components of physical therapy are critical. Learning proper body mechanics, posture, and strategies to avoid aggravating the pain can empower individuals to manage their condition more effectively.
Working with a licensed physical therapist ensures that these techniques are applied safely and effectively. Personalized treatment plans can make a meaningful difference in the quality of life for those suffering from neuropathic pain.
The role of psychotherapy in pain management
Psychotherapy can play a critical role in the management of neuropathic pain. This approach focuses on the psychological aspects of pain, helping individuals cope with the emotional and mental challenges associated with chronic discomfort. One common form of therapy used is cognitive-behavioral therapy (CBT).
CBT aims to change negative thought patterns that can exacerbate pain. By teaching patients how to reframe their thoughts, they can develop healthier coping strategies. This method focuses on breaking the cycle of pain and depression, reducing stress, and improving mental well-being.
Mindfulness techniques are also beneficial. Practices such as meditation and relaxation exercises can help individuals focus on the present moment, reducing anxiety and promoting relaxation. Mindfulness can alter their perception of pain, making it easier to manage.
Another valuable component is supportive psychotherapy. This type of therapy provides emotional support and validation, helping individuals express their feelings related to their pain. Having a safe space to discuss their experiences can lead to better emotional health and resilience.
Incorporating educational components in psychotherapy is essential. Patients can learn about the nature of pain, the brain’s response to pain signals, and the importance of managing stress. This knowledge empowers individuals to take an active role in their pain management.
Overall, psychotherapy offers a holistic approach that complements medical treatments for neuropathic pain, providing individuals with tools to improve their quality of life.
Alternative therapies for neuropathic pain

Alternative therapies offer additional options for managing neuropathic pain. Many people seek these methods when conventional treatments do not provide adequate relief. One popular alternative is acupuncture. This ancient practice involves inserting thin needles into specific points on the body to stimulate nerves and promote healing. Many patients report significant improvements in their pain after acupuncture treatments.
Herbal remedies are also commonly used. Certain herbs, like canabidiol (CBD) oil and turmeric, are thought to possess anti-inflammatory properties that can help reduce pain. However, it is important to consult with a healthcare provider before trying these treatments to ensure they are safe and appropriate.
Chiropractic care can provide relief for some individuals suffering from neuropathic pain. Chiropractors focus on spinal alignment and mobility, which can help alleviate pain and improve function. Regular adjustments may contribute to long-term pain management.
Physical activities like yoga and tai chi are beneficial as well. These practices encourage gentle movement, which can help enhance flexibility, reduce stress, and promote relaxation, all of which can help manage pain. The mind-body connection in these activities may improve an individual’s overall sense of well-being.
Additionally, biofeedback is a technique that teaches individuals how to control physiological functions. By learning to manage stress responses and muscle tension, patients can decrease their pain levels over time.
While alternative therapies can be effective, they should be seen as complementary to traditional treatments. Collaborating with healthcare professionals ensures that all facets of pain management are addressed.
How lifestyle changes can alleviate symptoms
Lifestyle changes can significantly help alleviate the symptoms of neuropathic pain. By adopting healthier habits, individuals can enhance their quality of life and potentially reduce pain levels. One important change is maintaining a balanced diet. Consuming a variety of fruits, vegetables, whole grains, and lean proteins can support overall health and aid in nerve function.
Regular physical activity is another key component. Engaging in moderate exercise, such as walking, swimming, or cycling, can improve blood circulation and release endorphins, which are natural pain relievers. It’s essential to choose activities that are enjoyable to ensure consistency.
Additionally, managing stress plays a crucial role in pain management. Chronic stress can amplify pain sensations. Techniques such as meditation, deep breathing exercises, or yoga can help reduce stress levels, promoting relaxation and potentially easing discomfort.
Getting adequate sleep is vital as well. Sleep deprivation can worsen pain and affect overall health. Establishing a regular sleep routine, creating a comfortable sleep environment, and minimizing electronics before bedtime can improve sleep quality.
Avoiding harmful habits is equally important. Reducing or eliminating alcohol and quitting smoking can positively impact nerve health and overall well-being. Both substances can worsen pain symptoms and hinder recovery.
Lastly, staying hydrated is crucial. Drinking enough water throughout the day supports nerve function and helps maintain bodily systems. Overall, making these lifestyle changes can create a positive impact on managing neuropathic pain and enhancing well-being.
Using hot and cold therapy for pain relief

Using hot and cold therapy is a simple yet effective method for alleviating neuropathic pain. Both hot and cold treatments work by affecting blood flow and nerve activity in the body, providing relief in different ways.
Heat therapy involves applying warmth to the affected area. This can be accomplished using heating pads, warm towels, or hot water bottles. The heat increases blood circulation to the area, promoting healing and relaxation of muscles. It is particularly useful for reducing stiffness and improving flexibility in muscle and joint tissues.
Heat therapy is best used for chronic pain conditions. If someone experiences ongoing discomfort due to nerve damage, applying heat can provide soothing relief. However, caution should be exercised to avoid burns by ensuring the heat source is at a safe, comfortable temperature.
On the other hand, cold therapy involves using ice packs or cold compresses. Cold therapy works by numbing the area and reducing inflammation. It helps to constrict blood vessels, which can decrease swelling and alleviate sharp pain sensations. Cold therapy is particularly effective for treating acute injuries or flare-ups of chronic pain.
When using cold therapy, it’s essential to protect the skin by wrapping ice packs in a cloth. Applying cold directly to the skin for too long can cause frostbite or skin irritation.
Knowing when to use heat or cold therapy is crucial. Generally, cold therapy is recommended during the first 48 hours after an injury or acute flare-up, while heat therapy is beneficial for chronic pain management. Combining both therapies can offer versatile pain relief strategies for individuals dealing with neuropathic pain.
Exploring dietary impacts on nerve health
Diet plays a crucial role in maintaining nerve health and can significantly impact neuropathic pain. Certain nutrients are essential for nerve function, while others may help reduce inflammation. A balanced diet rich in vitamins and minerals is vital for overall health and well-being.
Vitamin B12 is particularly important for nerve health. It helps maintain the myelin sheath, which protects nerve fibers. A deficiency in vitamin B12 can lead to nerve damage, resulting in symptoms like numbness and tingling. Foods high in B12 include meat, fish, eggs, and dairy products.
Another beneficial nutrient is omega-3 fatty acids. These healthy fats, found in fish like salmon, walnuts, and flaxseeds, can help reduce inflammation and support nerve repair. Including more omega-3 fatty acids in the diet may improve nerve function and alleviate pain symptoms.
Antioxidants also play a significant role in nerve health. Foods rich in antioxidants, such as berries, green leafy vegetables, and nuts, can protect nerves from oxidative stress and damage. These foods help reduce inflammation and promote healing.
Additionally, a diet low in processed sugars and saturated fats can be beneficial. High sugar intake may worsen inflammation, leading to increased pain levels. Focusing on whole, unprocessed foods can help improve overall health and support nerve function.
Staying well-hydrated is equally important for maintaining nerve health. Drinking enough water aids in nerve function and overall body processes. Overall, by making dietary changes and focusing on nutrient-rich foods, individuals can positively impact their nerve health and potentially reduce neuropathic pain.
The importance of early diagnosis

The importance of early diagnosis in managing neuropathic pain cannot be overstated. Detecting this type of pain as soon as possible can lead to more effective treatment options and better outcomes. When neuropathic pain is identified early, healthcare providers can implement treatments that may prevent further nerve damage and alleviate symptoms more effectively.
One key reason early diagnosis matters is that it can help differentiate neuropathic pain from other types of pain, such as nociceptive pain. Understanding the specific type of pain allows healthcare professionals to tailor treatment plans that target the underlying causes rather than just masking symptoms.
Additionally, early intervention often results in a better quality of life for patients. When neuropathic pain is addressed promptly, patients may find relief sooner, which can reduce the physical and emotional burden associated with chronic pain. Managing pain early can also help prevent issues like anxiety and depression that often accompany long-term pain conditions.
Another benefit of early diagnosis is the opportunity for patients to make lifestyle changes that can positively affect their health. With a proper diagnosis, individuals can modify their diet, engage in physical activity, and adopt other healthy habits that support nerve health and overall well-being.
Early diagnosis also allows for more comprehensive monitoring. Regular follow-ups with healthcare providers ensure that treatment plans are adjusted as needed and that any new symptoms are addressed quickly. This approach can lead to better long-term management of neuropathic pain.
In summary, recognizing and diagnosing neuropathic pain early is crucial for effective management, improving quality of life, and minimizing long-term complications.
Understanding chronic vs. acute neuropathic pain
Understanding the differences between chronic and acute neuropathic pain is essential for effective pain management. These two types of pain have distinct characteristics and may require different approaches to treatment.
Acute neuropathic pain is typically short-term and often arises suddenly due to an identifiable cause, such as an injury or infection. This type of pain usually resolves as the underlying issue heals. For example, if someone suffers nerve damage from a recent surgery, the pain felt in the weeks following the procedure may be classified as acute.
In contrast, chronic neuropathic pain persists for a longer duration, usually defined as lasting more than three months. This type of pain can develop gradually and may not have a clear initial cause. Conditions such as diabetes, multiple sclerosis, or even phantom limb pain can lead to chronic neuropathic pain. It often becomes a complex condition, involving a series of symptoms that can significantly impact a person’s quality of life.
Another critical difference is how pain is experienced. Acute pain tends to be sharp and intense, often described as a sudden jolt. Chronic pain, however, may vary in character. Individuals may experience burning, tingling, or constant dull aches, which can fluctuate in intensity over time.
Diagnosis for each type of pain also varies. While acute neuropathic pain might be recognized quickly based on recent injury history, chronic neuropathic pain often requires thorough investigation, including patient history, imaging studies, and other diagnostic tests to uncover underlying conditions.
Understanding the differences between acute and chronic neuropathic pain is important for patients and healthcare providers alike. It helps in developing effective treatment plans that can address symptoms and improve overall health.
In Conclusion: Understanding and Managing Neuropathic Pain
Neuropathic pain can be a challenging condition that affects many individuals. Understanding the differences between acute and chronic neuropathic pain is essential for effective management. Early diagnosis and tailored treatments can make a significant difference in a person’s quality of life.
Incorporating lifestyle changes, such as a balanced diet, regular exercise, and stress management techniques can help in alleviating symptoms. Additionally, exploring various treatment options, including medications, physical therapies, and alternative therapies, allows individuals to find the relief they need.
Living with neuropathic pain can be difficult, but with the right knowledge and support, individuals can navigate their journey toward improved health and well-being.
FAQ – Frequently Asked Questions about Neuropathic Pain
What is neuropathic pain?
Neuropathic pain is a type of pain that occurs due to damage or dysfunction of the nerves. It often manifests as burning, tingling, or shooting sensations.
What are the main causes of neuropathic pain?
Common causes include diabetes, multiple sclerosis, shingles, spinal injuries, and certain medications.
How can lifestyle changes impact neuropathic pain?
Adopting a balanced diet, engaging in regular physical activity, managing stress, and staying hydrated can help reduce symptoms and improve overall nerve health.
What are some effective treatments for neuropathic pain?
Treatments can include medications like antidepressants and anticonvulsants, physical therapy, hot and cold therapies, and alternative therapies like acupuncture.
Why is early diagnosis important for neuropathic pain?
Early diagnosis allows for timely intervention, which can prevent further nerve damage and improve treatment effectiveness, leading to a better quality of life.
How can I differentiate between acute and chronic neuropathic pain?
Acute neuropathic pain is short-term and often linked to an identifiable cause, while chronic neuropathic pain persists for longer than three months and may not have a clear origin.




